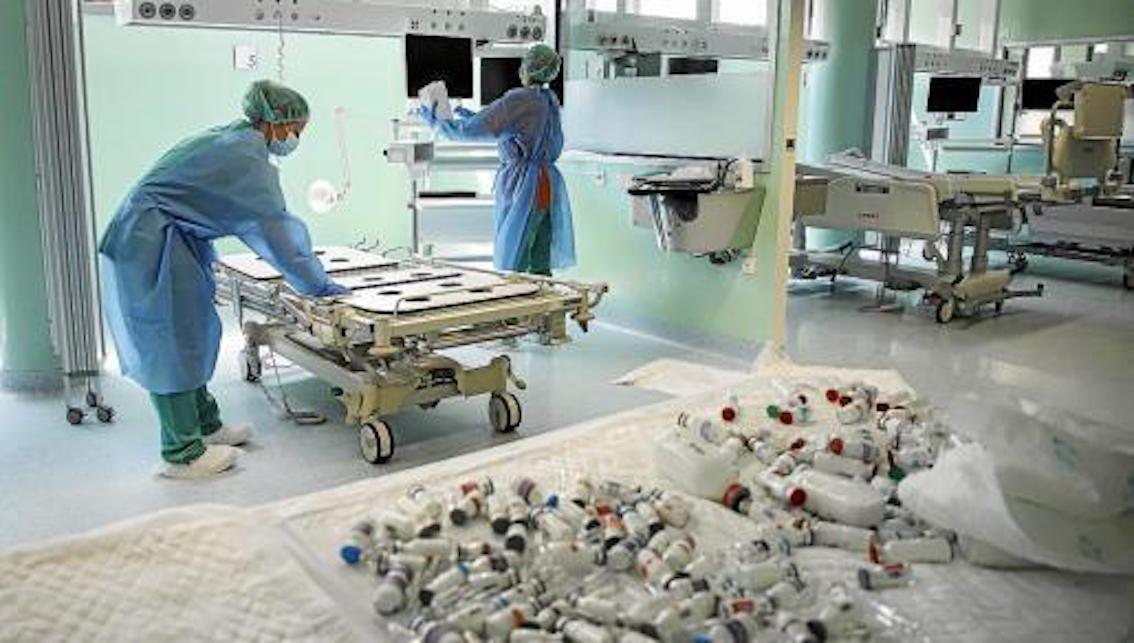
Beds, 5 litre cans of bleach and other materials are stacked and ready in the corridors as the 18-bed ICU is split in two with 8 isolated places, just in case they’re needed in future.
The seriously ill coronavirus patients continue to be cared for in a former post-anesthetic unit, called URPA, which has eight beds, all of which are currently occupied.
"The number of Covid-19 patients has been declining so now we can bring both units together as a single area,” explained Dr Gemma Rialp, Head of Son Llàtzer ICU.
Once the ICU is disinfected, there will be 8 beds available for coronavirus patients and 20 for other patients, but no-one is allowed in just yet.
“We cannot admit anyone for 48 hours so we had to transfer patients to other hospitals like Inca because Son Espases doesn’t have any places available for non-COVID patients.”
De-escalation
The hospital is reorganising in an attempt to return to normality but bearing in mind coronavirus is here to stay.
"We expect a rebound next week, with an influx of more patients, so our planning must be conscientious and prudent,” warned Dr Rialp.
Son Llàtzer’s first coronavirus patient was admitted on March 13.
"It has been a tough month in terms of healthcare pressure with a lot of involvement from doctors, nurses, assistants, anaesthetists, caretakers, cleaners, IT and maintenance. Everyone here has done a tremendous job," she said.
Dr Rialp says the de-escalation has only been possible because people have stayed home and fewer people were infected, but said it’s essential to keep our guard up.
“This virus lasts for two or three weeks and we can't predict what might happen, it's not like the flu,” she said.
The Son Llàtzer ICU was more than 70% full during the acute phase of the pandemic and at its highest peak there were 25 patients.
"We have had more than Son Espases, especially at the beginning, and we had a terrible time because our architecture and modules are not comparable so we had to expand by taking space from other units," she says.
Family Visits
Until now, most Covid-19 patients could only communicate with family via video-conference and were allowed access to say goodbye to patients who were dying.
Family members can now request a visit and the staff at each Hospital or Health Centre will be in charge of managing requests, planning visits, explaining the procedure and supplying protective clothing.
A maximum of two people per patient is allowed in alternating shifts and Healthcare Professionals recommend that visits do not exceed 30 minutes.

No comments
To be able to write a comment, you have to be registered and logged in
Currently there are no comments.